TeleportScienceNav
Biomarker Discovery
Different definitions of biomarkers have been suggested (e.g. NIH Biomarker Definitions Working Group), but all point out that they reflect the dynamic nature of physiological and pathological procedures in biologic systems. In the proteomics filed of activity numerous studies were published describing the discovery of putative biomarkers using mass spectrometry. Although these studies established a trend-setting basis for mass spectrometry in biomarker research, they also initiated a controversial debate questioning the clinical validity of the obtained results. In fact, very few, if any, new biomarkers have been established through the proteomics process chain of discovery and identification, validation in clinical trials, and approval by regulatory agencies.

The figure depicts the different phases and estimated timelines for the discovery and validation of biomarkers.
Types of Biomarkers
Prognostic Biomarker :
capable of providing information on clinical outcome at the time of diagnosis, independent of therapy.
Predictive Biomarker :
capable of providing information on the likelihood of response to a given therapeutic modality. Such markers are either within the target of the treatment, or serve as modulators or epiphenomena related to expression and/or function of the target.
Screening Biomarker :
capable of providing information on clinical diagnosis in (general) population.
Transition
The number of candidates derived from the discovery phase should be limited because the validation of these candidates otherwise exceeds a feasible validation design. Nevertheless, only few – if any - new biomarkers have been established so far by finishing the proteomics process chain of discovery and identification, validation in clinical trials, and approval by regulatory agencies. Prior to clinical validation (e.g. determination of the positive predictive value) and even more for clinical implementation of a peptide biomarker the conversion from the multiplex system to a monoplex system is required. Unique and general considerations in developing anti-peptide immunoassays are requirements for elimination of assay cross-reactivity with the protein precursors. Emerging alternatives are a broader application of mass spectrometry in clinical laboratories, or the development of techniques, which combine the specificity of mass spectrometry with the sensitivity of antibody based methods.

The figure shows the transition of assay systems from discovery to validation/application.
Prototype Assay
A prototype assay allows for absolute quantification of a given peptide of interest using mass spectrometry. To achieve the quantification of a specific peptide, isotopic labelled peptides (peptides that are identical to the specific peptide but posses different masses due to the presence of isotopes) are added prior to sample processing. By calculating the ratio between the peptide of interest and the isotopic counterparts (that have a known concentration) the amount of the peptide of interest can be calculated.

Validation
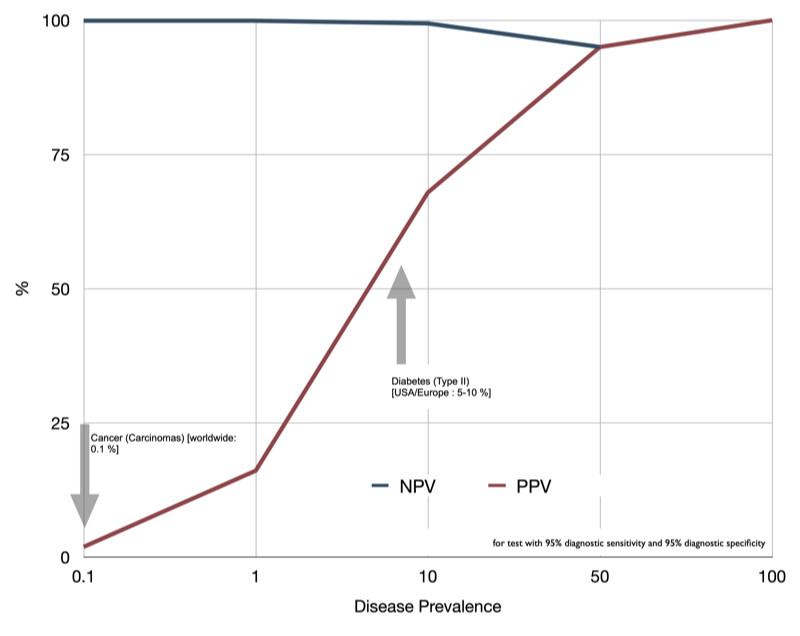
The development of new biomarkers consists essentially of a discovery and a validation phase. The extraordinary challenge of biomarker discovery is to obtain markers with sufficient predictive values and not only the validity of the test system or intrinsic biochemistry itself. Consequently, an important point for consideration in biomarker research is that sensitivity and specificity in discovery studies are determined in selected cohorts with a high prevalence of the respective disease. In a routine clinical setting, however, the disease prevalence will be much lower. It is not important to know the probability of a positive test if the disease is present but to know the probability of the presence of the disease if the test is positive. This probability depends on the prevalence of the disease and refers to the positive predictive value (PPV). The PPV is the probability in case of a positive test, that the patient really has the specified disease.
Requirements for Implementation
Regardless of the type of biomarker to be investigated, in order for a biomarker to be considered for routine implementation it needs to be demonstrated that measurement of the marker ultimately impacts on clinical management of the malignant disease, either by improving patient outcome or quality of life or by lowering cost of care.